While I agree with Professor Singer that saving a lone yachtswoman last week was well worth it (Sunday Age, 8/1/95), I am concerned that the examples used to support his argument were misleading.
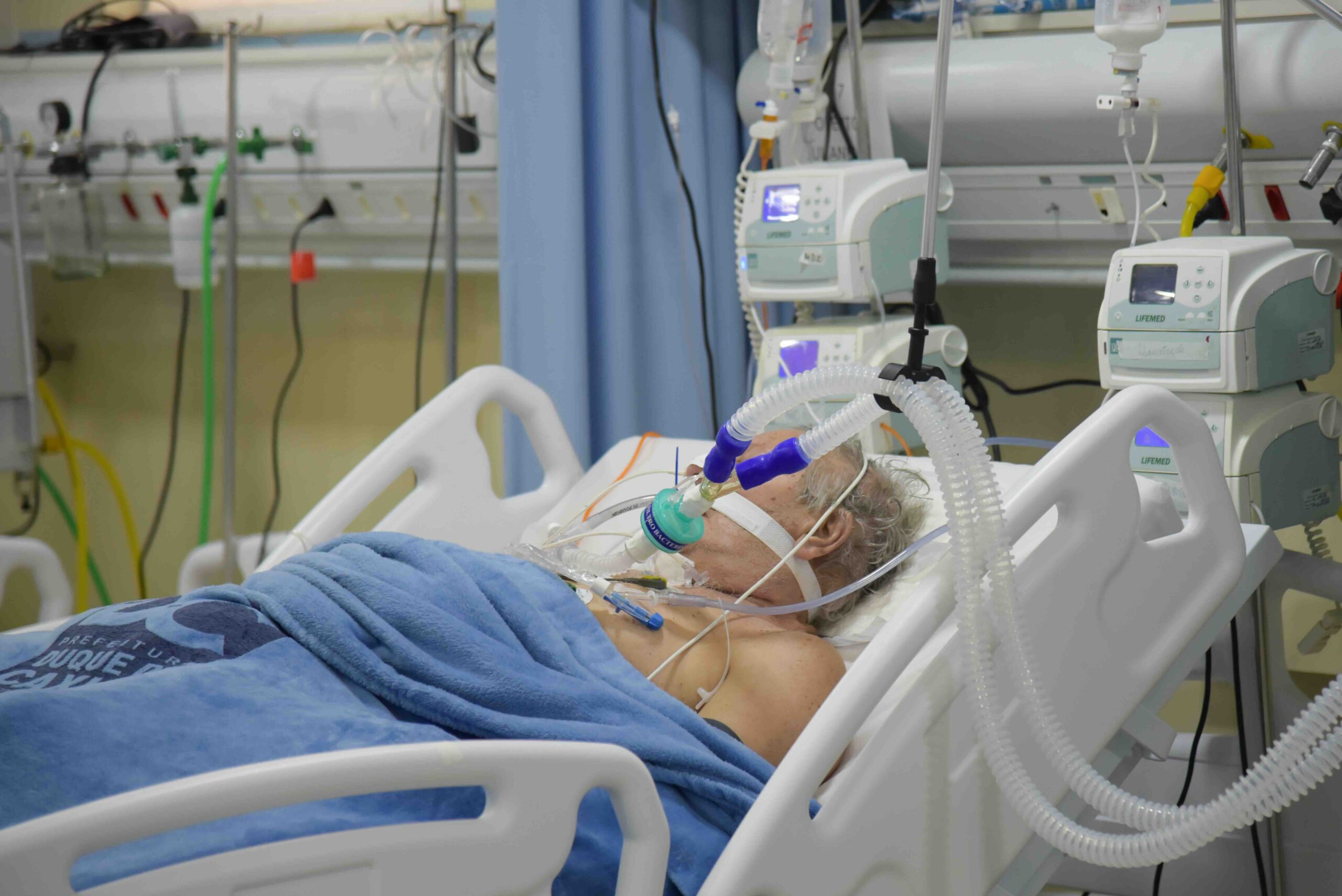
One of his examples was an Intensive Care Unit in Melbourne where “many patients who would be helped by intensive care” were turned away. Singer predicts that “some of these patients will die, when with intensive care they would have lived”. My question to Singer is: how long would these patients have lived and with what quality of life?
Professor Singer seems to think that the most expensive type of medical treatment (eg the sophisticated technology available in an Intensive Care Unit or the latest drug) is necessarily the best type of medical care. Often this is simply not the case.
The past 20 years has seen a significant increase in investment in life-saving technologies. In fact, Intensive Care Units are being used more often and with less discrimination now than ever before.
Whether this investment in increasingly expensive and sophisticated medical technology has improved patients’ well-being, or merely supported a burgeoning medical industry and bolstered medical egos, is largely unknown. I find it alarming that there has been no attempt by the Health Department to obtain such data.
There has not been an adequate analysis of the overall impact of the sophisticated medical technologies on patients’ recovery after treatment in an Intensive Care Unit. Often the only information available is whether a patient was discharged from the unit alive or dead.
It is unreasonable to expend a significant proportion of the health care budget on Intensive Care Units without knowing who does and who does not benefit from such an investment. At least when money is spent on rescuing those lost at sea or in the bush, for example, we are reasonably confident of the outcome.
First published as a Letter to the Sunday Age 15 January 1995